Leg ulcers are an excavation of the skin surface that occurs when inflamed necrotic tissue sloughs off. A majority of reported leg ulcers occurs as a result of chronic venous insufficiency. Moreover, other factors that contribute to the development of the ulcerations brought about by lesions are due to arterial insufficiency, partial and full thickness burns, sickle cell anemia and other pathological factors.
Leg ulcers can either be arterial or venous in nature. Chronic arterial disease is characterized by intermittent claudicating pain caused by strenuous activity that are generally relieved by rest. On the other hand, chronic venous insufficiency is characterized by pain described as aching or heaviness. Arterial ulcers are typically small, circular and deep ulcerations in the tips of the toes or in the web spaces between the toes. Venous ulcers occur in the area of the medial and lateral malleolus area and generally seen in patients with venous hypertension in which this type of ulceration being painless in nature.
Pathophysiology of leg ulcers
Leg ulcers occur when there is an inadequate exchange of oxygen and other nutrients in the tissue. There is an underlying metabolic abnormality which causes the onset of leg ulcers. When cellular metabolism cannot maintain and keep up with energy balance at the rate at which cell death outpace the production of new cells, cellular necrosis occurs. Alterations in the blood vessels of the arterial, capillary and venous levels may subsequently affect cellular process which leads to the formation of ulcers in the lower extremities.
Clinical manifestations of leg ulcers
The characteristics of leg ulcers are determined by the cause of the ulcer itself. Most ulcers, especially in the elderly patients have more than one pathologic cause. The symptoms are highly dependent on whether the problem is arterial or venous in origin. The severity of the symptoms depends on the extent of the duration of the vascular insufficiency. The ulcer itself appears as an open, inflamed sore and the area affected may have purulent discharges covered by a dark hard crust. Furthermore, untreated ulcerations of the leg can lead to serious gangrenous infection resulting from severe arterial or venous ischemia.
General medical management of leg ulcers
Individuals with leg ulcers can be effectively managed by consistent wound care and antibiotic therapy since all ulcers in general have the potential to become infected. Antibiotic therapy is normally prescribed when the ulcer is infected and the specific antibiotic agent is to be ideally based on the patient’s individual culture and sensitivity results. Oral antibiotics are normally prescribed since topical antibiotics are not fully proven to be as an effective remedy for treating full blown infected leg ulcers.
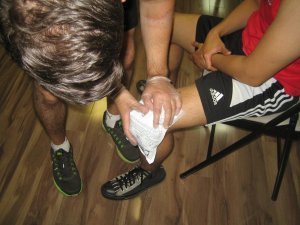
Wound dressing is very important in keeping the leg ulceration free from infection. After the circulatory status has been determined, and depending on the technique used by the physician or nurse, the simplest method is usually to use a wound contact material such as a sterile gauze to cover the wound bed of the leg ulcer .
Excerpt
The primary pathologic cause of leg ulcers needs to be addressed
first in order for proper wound healing to occur. Promoting adequate nutrition and improving physical mobility are important supplementary health teachings and the rest of the members of the healthcare team can impart to the patient towards faster wound healing. Furthermore, to promote wound healing, measures to maintain the sterility of wound dressing technique and proper medication compliance are essential components in effectively treating leg ulcers.

